
The first time my cycle went completely off the rails, I didn’t think it was a big deal. A late period here, crushing cramps there, fatigue that sat on my chest like something I couldn’t shake. I kept waiting for it to regulate on its own. It didn’t.

If you’re looking to learn holistic hormonal balance for women, the most honest thing I can tell you is that it isn’t one fix — it’s a sequence. Hormonal health responds to a layered system: what you eat, how you move, what you’re exposed to, how you manage stress, when you test, and what you supplement. When those elements work together, cycles regulate, fertility improves, and symptoms that felt permanent start to ease.
- This approach works best if you’ve already ruled out acute medical emergencies and want to reduce symptoms through root-cause changes, not just symptom suppression.
- Expect real traction in 3–6 months if you apply the steps consistently — hormones respond slowly, but they do respond.
- Who this is actually for: women with PCOS, endometriosis, fibroids, thyroid issues, irregular cycles, PMS, or anyone who’s been told “your labs are normal” while still feeling anything but.
What Holistic Hormonal Balance Actually Means
Holistic hormonal balance for women means treating the endocrine system as an ecosystem, not a single broken part. Estrogen, progesterone, insulin, cortisol, and thyroid hormones don’t operate in isolation — they speak to each other constantly. When one is elevated or suppressed, others shift to compensate, and that cascade is usually what creates the symptoms women experience: heavy bleeding, skipped cycles, mood swings, infertility, and fatigue that no amount of sleep fixes.
The natural approach differs from conventional hormone therapy in that it targets the upstream causes — diet, toxic load, stress, blood sugar dysregulation — rather than replacing or suppressing hormone output directly.
| Approach | Target | Timeline | Side Effects |
|---|---|---|---|
| Conventional hormone therapy | Symptom suppression | Immediate | Possible (mood, clots, dependency) |
| Holistic / natural approach | Root cause correction | 3–6 months | Minimal when done correctly |
| Combination approach | Acute + long-term | Varies | Depends on medications used |
Three Things That Surprised Me About Hormones
- Blood sugar instability is a bigger driver of hormonal chaos than most women ever get told.
- You can have “normal” TSH and still have thyroid-related cycle disruption.
- The liver processes estrogen — if it’s overloaded, excess estrogen recirculates and worsens symptoms.
How Long Does It Actually Take?
| Stage | What Happens | Estimated Time |
|---|---|---|
| Foundation (Steps 1–2) | Understanding your cycle, cleaning up diet | Weeks 1–3 |
| Energy + Mindset (Steps 3–4) | Adding energy medicine, reflection practices | Weeks 4–6 |
| Environment (Step 5) | Reducing toxin exposures in home and body products | Weeks 5–8 |
| Metabolic reset (Step 6) | Stabilizing blood sugar and insulin patterns | Weeks 6–10 |
| Testing + Supplements (Steps 7–8) | Running labs, introducing targeted supplements | Weeks 8–14 |
| Cycle fluency (Step 9) | Accurately reading and timing your cycle | Month 3–4 |
| Movement integration (Step 10) | Exercise calibrated to your hormonal phase | Month 3–6 |
| Total | Full system integration | 3–6 months |
Order matters more than speed here — trying to supplement before you’ve stabilized blood sugar is like patching a roof in a rainstorm. And if you’re moving slower than this estimate, that’s not failure — hormones shift gradually, and the women who try to rush the process usually plateau faster.

Starting With What You Eat — And Why Food Comes First
The first thing most women do when they decide to fix their hormones is buy supplements. I did it too. I spent money on adaptogens before I’d fixed the fact that I was eating refined carbs twice a day and skipping breakfast so often my cortisol was spiking before 9am.
Food is Step 2 for a reason — it’s the medium in which everything else operates. Cruciferous vegetables support estrogen metabolism through a process in the liver. Healthy fats are the literal building blocks of steroid hormones. Fiber binds to excess estrogen in the digestive tract and escorts it out before it can be reabsorbed. None of this is complicated, but it requires specificity. Not just “eat healthy” — eat in a way that reduces your toxic estrogen load, feeds the liver’s detox pathways, and keeps blood sugar stable between meals.
The recipes that made the most difference weren’t trendy. They were consistent. Protein at every meal. Seeds cycled across the month to mirror estrogen and progesterone phases. Leafy greens daily. Less alcohol, less sugar, more fat than I’d ever let myself eat before. When food becomes your baseline, everything added after it — supplements, energy medicine, exercise — lands harder.

Energy Medicine Isn’t What I Expected It to Be
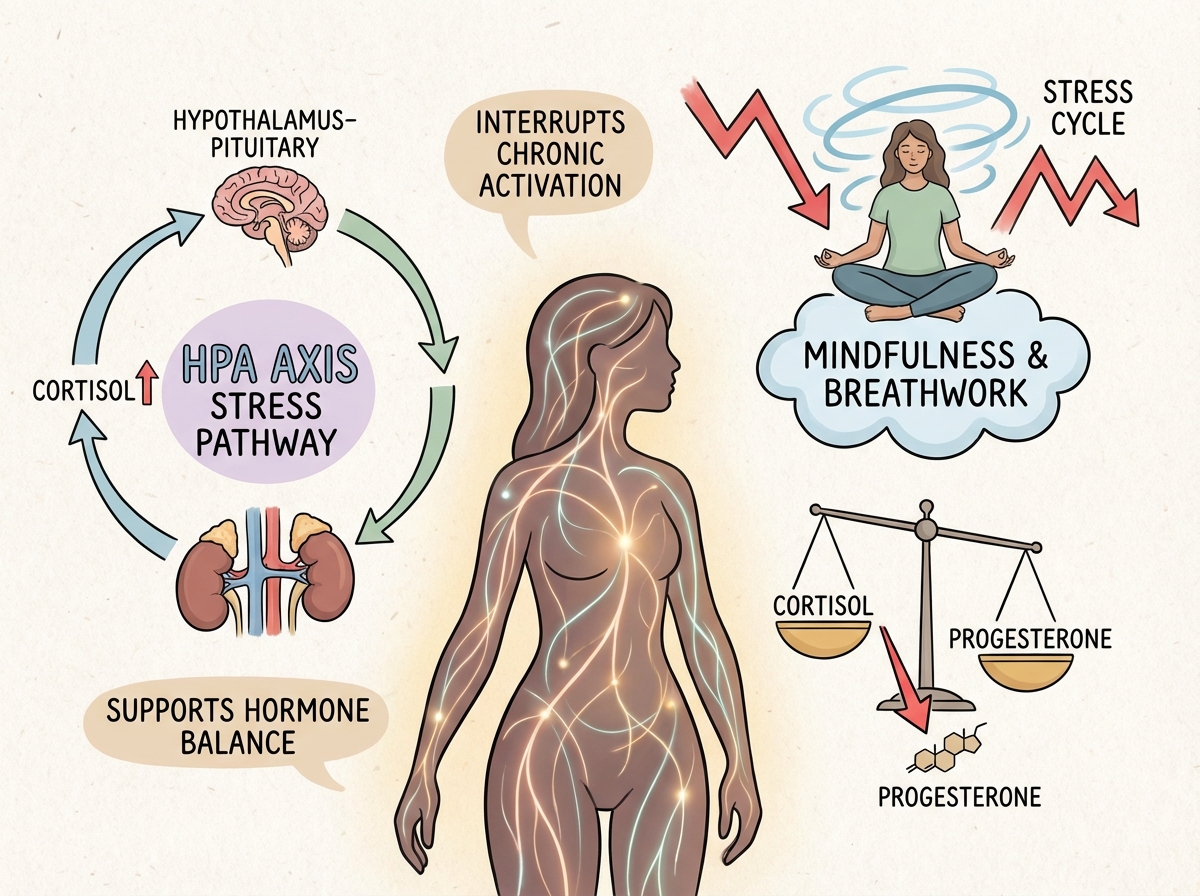
I’ll be honest — “energy medicine” was where I almost checked out. It sounded like the kind of thing that belonged on a wellness influencer’s story, not in a serious protocol for hormonal health. But tai chi, acupressure, and specific breathing techniques have measurable effects on the nervous system, and the nervous system is intimately connected to the HPA axis — the hormonal command center that governs cortisol, which governs almost everything else.
The specific realization that shifted my thinking was this: chronic low-grade stress doesn’t feel dramatic. It doesn’t feel like anxiety. It feels like being slightly “on” all the time — a hum of vigilance that never fully turns off. That hum suppresses progesterone production, raises cortisol, and tells your body that now is not a good time to ovulate. Energy practices — even five minutes of structured breathwork in the morning — are not spiritual add-ons. They’re inputs into a physiological system that is deeply sensitive to perceived safety.
Acupressure points that correspond to reproductive organs have been used in traditional Chinese medicine for thousands of years. Whether you approach that from a skeptical or open perspective, the practices themselves are low-risk, inexpensive, and consistently reported to reduce pain and improve cycle regularity in women with dysmenorrhea and anovulatory cycles.
The Reflection Step That Most Women Skip Entirely
Step 4 — reflection — is the one I see skipped most often, and I understand why. It feels soft compared to running labs or adjusting supplements. But the women who make the fastest progress are usually the ones who get honest about the mental and emotional patterns that are running underneath the physical symptoms.
Stress doesn’t have to be catastrophic to be hormonally disruptive. A perfectionistic approach to work, a relationship that keeps you in a low-level state of emotional hypervigilance, a deep history of body distrust — these things create a nervous system that is chronically in a state of low-grade alarm. Progesterone drops. Cortisol stays elevated. Cycles become irregular. And no supplement fixes that.
Mindfulness isn’t meditation as a productivity hack. In this context, it’s a way of developing the capacity to notice what the body is actually communicating — fatigue before it becomes collapse, anxiety before it becomes insomnia — so that you can respond rather than push through. The women I know who learned to track their emotional landscape alongside their physical cycle found the intersection revealing in ways that made every other step sharper.
Toxins You Haven’t Thought About Yet
This is where I lost a few hours of my life reading labels for the first time. Endocrine-disrupting chemicals — phthalates in plastic containers, BPA in receipts and packaging, parabens in skincare, synthetic fragrances in nearly everything — mimic or block estrogen signaling. They’re not dramatic poisons. They accumulate.
The biggest mistake people make when approaching toxin reduction is going all-in immediately, throwing out every product in the bathroom in one afternoon, and then burning out on the overwhelm. The practical version is far more manageable: prioritize swaps in the categories with highest daily exposure. Body lotion and deodorant are on your skin for hours. Cookware and food storage are touching your food. Tampons and pads are used internally. Start there, then expand outward.
Swapping to fragrance-free, paraben-free personal care products and glass or stainless steel food storage makes a measurable dent in daily chemical load without requiring a lifestyle overhaul. The goal isn’t purity — it’s reduction. Even modest reductions in daily endocrine disruptor exposure give the liver less work to do and the hormonal system a cleaner signal environment.

Blood Sugar Is the Hidden Lever
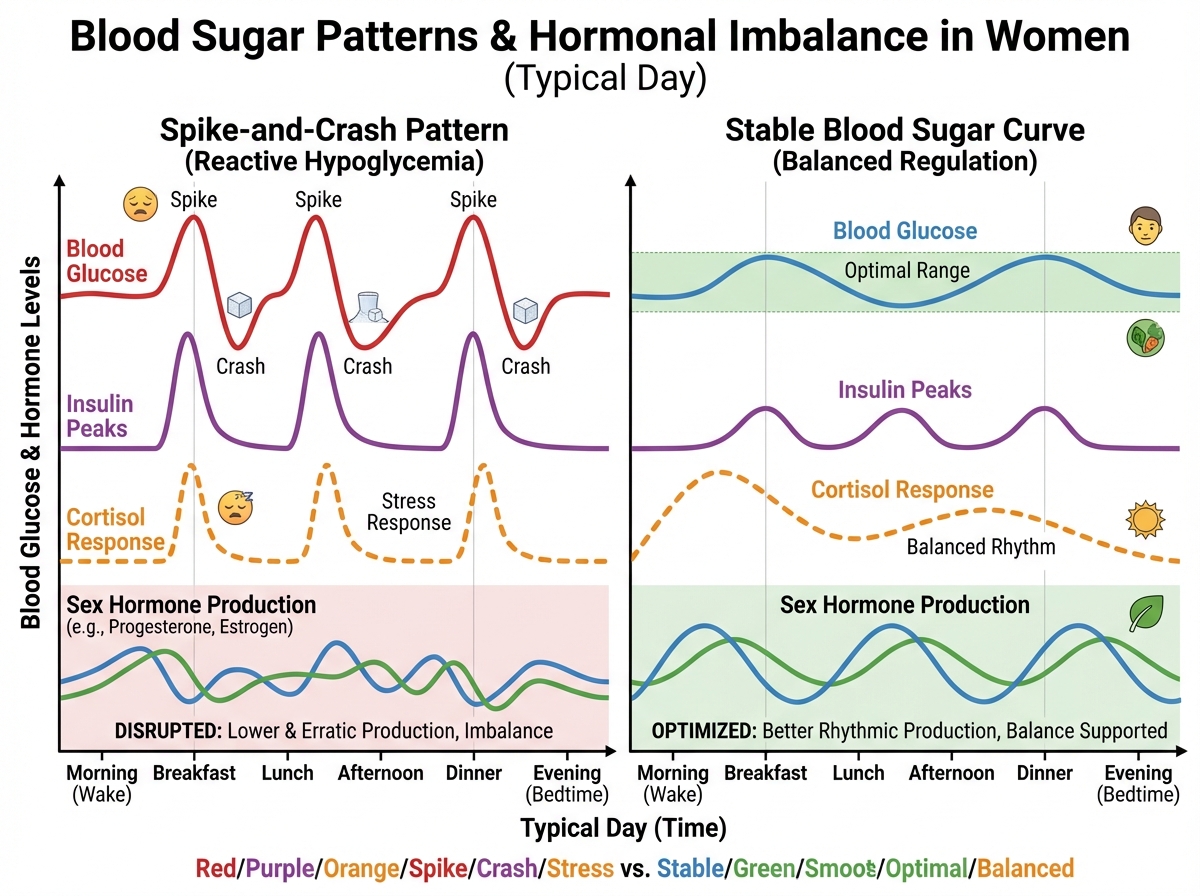
Step 6 stopped me cold the first time I really understood it. I didn’t have diabetes. I didn’t think insulin was my problem. But blood sugar dysregulation — the constant spike-and-crash pattern that comes from skipping meals, eating refined carbs, or going too long without protein — creates a hormonal environment that makes everything else harder to fix.
Insulin resistance, even in a mild, subclinical form, is one of the primary drivers of PCOS. It suppresses sex hormone-binding globulin (SHBG), which means more free testosterone circulates. It disrupts ovulation. It worsens estrogen dominance. And it’s extremely common in women who would never describe themselves as insulin-resistant because they’re not overweight or pre-diabetic by conventional metrics. If you’re learning natural ways to balance hormones and you haven’t addressed blood sugar, you’re working with one hand tied behind your back.
The intervention is not a keto diet. It’s protein at breakfast, fiber with every meal, avoiding the long fasted stretches that create cortisol spikes, and paying attention to how your energy feels two hours after eating. A continuous glucose monitor, even for a two-week experiment, is one of the most instructive tools a woman with hormonal symptoms can use. What you see on that graph explains a lot.
Labs, Supplements, and Why Order Matters
The biggest mistake people make when learning about hormonal health naturally is supplementing before they’ve tested. Guessing that you need progesterone, or iron, or vitamin D, or zinc without data is not holistic — it’s just unguided. The right labs, ordered at the right time in your cycle, tell a completely different story than a random hormone panel drawn on day 15 instead of day 21.
There are assessments you can complete before you even see a practitioner that help you identify where your imbalances are likely clustering — thyroid, adrenal, reproductive hormone, or metabolic. Those assessments inform which labs to prioritize, which is useful because running every possible test at once is expensive and often overwhelming to interpret. Once you have data, supplement selection becomes targeted: inositol and berberine for insulin resistance, vitex for progesterone support, NAC for PCOS inflammation, magnesium glycinate for sleep and cycle pain. Not all of those for everyone — only the ones the data supports.
The supplement industry does not reward your discernment. Brand quality matters enormously. Third-party testing, bioavailable forms, no unnecessary fillers — these differences are not marketing; they affect whether the supplement actually crosses into your cells or just passes through.
Cycle Tracking Is Not What Most Women Think It Is
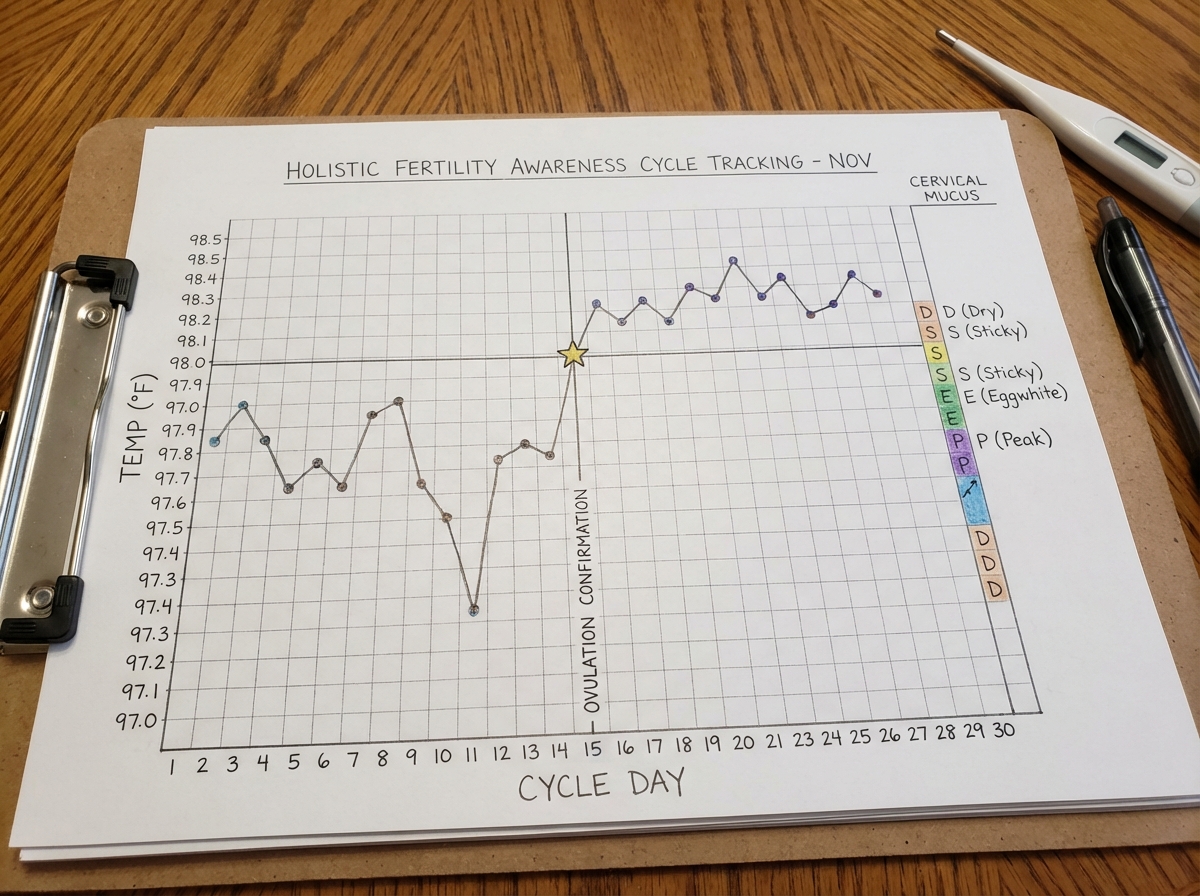
Most women who say they’re tracking their cycle are tracking the start date. That’s not cycle tracking — that’s record-keeping. Real cycle tracking, the kind that gives you fertility awareness, involves reading three distinct biological signs: basal body temperature (BBT), cervical mucus quality, and cervical position. Together, these signs confirm ovulation — not just predict it, but confirm it happened.
This distinction matters enormously whether you’re trying to conceive or trying to avoid pregnancy. An app prediction is a statistical average. Your actual cycle is not an average — it’s a reflection of your unique hormonal environment on that specific month, affected by sleep, illness, stress, and travel. When you learn to read your own signs, you stop depending on an algorithm to tell you what your body is already communicating directly.
The learning curve is real. The first two or three cycles you track feel like trying to read a language you don’t quite speak yet. Then something clicks. You notice the shift in mucus two days before the temperature rise. You recognize what an ovulatory chart looks like versus an anovulatory one. That knowledge is genuinely empowering in a way that no app shortcut can replicate.
Movement That Heals Instead of Stresses
The exercise advice that women with hormonal imbalances receive is often exactly wrong. High-intensity interval training, daily cardio, heavy lifting every session — these raise cortisol, and when cortisol is already elevated, more stress on the system deepens the problem rather than fixing it. Women with PCOS, adrenal dysfunction, or HPA axis dysregulation often feel worse after aggressive workout programs, not better, even when the scale moves.
Restorative yoga is not beginner yoga for people who aren’t fit enough to do “real” exercise. It’s a parasympathetic nervous system activator. Held poses with props, supported inversions, and long exhale breathing directly counteract the cortisol-dominant state that makes hormonal recovery difficult. Pairing restorative yoga with walking, swimming, or gentle strength training calibrated to your cycle phase gives the body the stimulus it needs without the hormonal blowback.
Tennis ball massage — rolling the fascia around the hips, sacrum, and lower back — sounds like a footnote. It isn’t. The pelvic fascia holds chronic tension that reduces circulation to the reproductive organs. Releasing that tension regularly has a real, felt effect on pelvic pain and cramping that women with endometriosis and fibroids report noticing faster than most other interventions.
What I’d Do Differently From the Start
Looking back at the beginning of this process, the biggest time-wasters were trying to fix symptoms individually instead of building the system, and supplementing before I had data. The breakthroughs came when I stopped treating each symptom as a separate problem and started understanding them as signals from a single ecosystem.
Eat protein at your first meal, every day. It stabilizes cortisol from the moment you wake up and prevents the blood sugar crash that drives afternoon cravings and hormonal chaos.
Track your basal body temperature before you do anything else. Two weeks of BBT data tells you more about what’s happening in your cycle than most standard blood panels ordered at the wrong time.
Swap your five highest-exposure personal care products first. Deodorant, body lotion, shampoo, cookware, and food storage — reduce your endocrine disruptor load in the places that matter most before perfecting everything else.
Run labs at the right time in your cycle. Progesterone is meaningless tested on day 5. Request your panel specifically on day 21 of a 28-day cycle, or 7 days after confirmed ovulation.
Add breathwork before you add supplements. Five minutes of extended exhale breathing in the morning costs nothing, directly lowers cortisol, and creates a more receptive environment for every supplement you take afterward.
Seed cycle for at least one full menstrual cycle before judging it. One month of flaxseed and pumpkin seed in the follicular phase and sesame and sunflower in the luteal phase isn’t enough. Give it three before drawing conclusions.
Do not train hard during the luteal phase if you’re symptomatic. The second half of your cycle requires more recovery. High-intensity training in that window when your hormones are already strained adds to the burden, not to the benefit.
Interpret your labs with your symptoms, not in isolation. A TSH of 2.5 might be fine for one woman and symptomatic for another. Learn the functional reference ranges, not just the lab’s flagged ranges, and notice whether the numbers match how you actually feel.

Leave a Reply