Most people get their first real lower back pain episode and immediately stop moving. That instinct — to rest, to wait it out, to protect the area by doing nothing — feels right. It is almost always wrong.
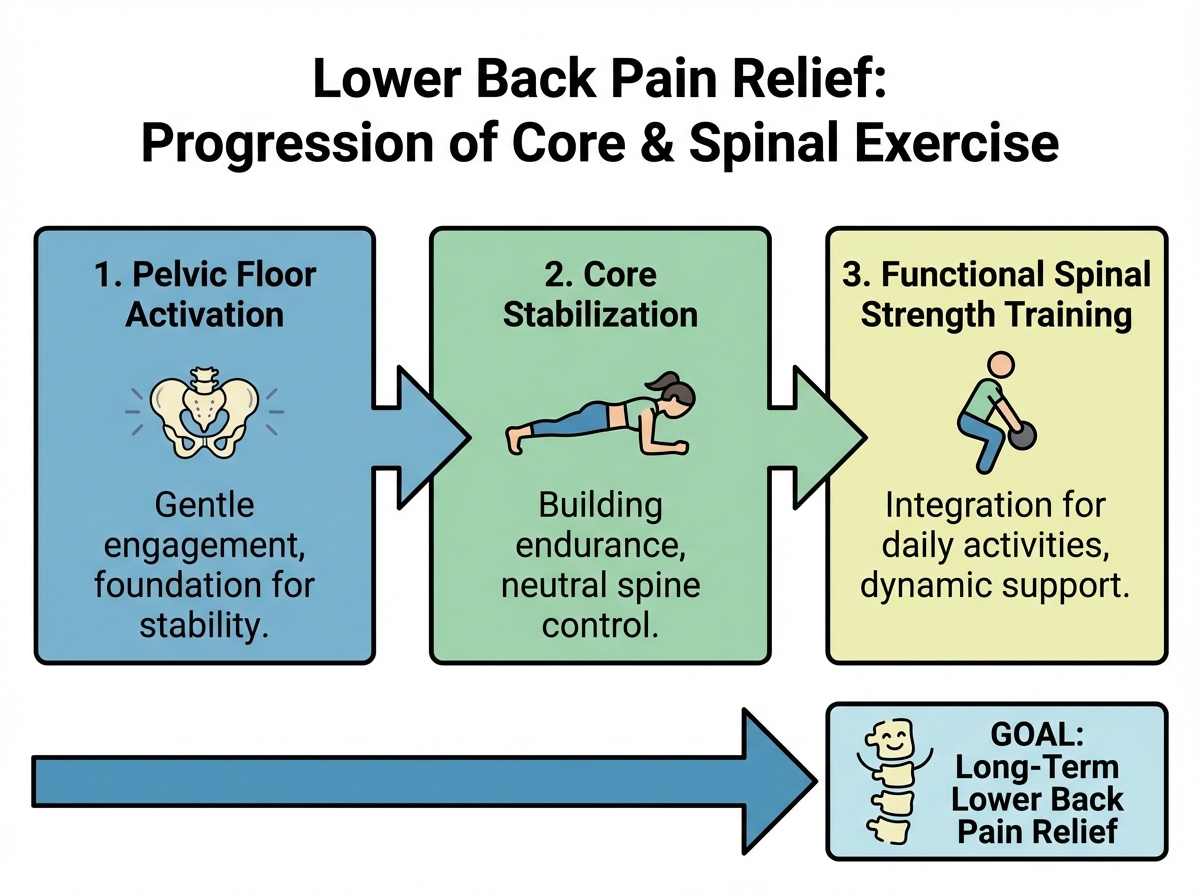
If you’re looking to learn lower back pain relief through exercise, the most effective approach is not stretching the pain away or grinding through generic gym routines. It’s reactivating the deep stabilizer muscles that your body quietly switched off — often long before the pain started. Core stabilizer training, done in the right sequence and at the right intensity, addresses the actual structural problem: a spine that has lost the muscular support it needs to move without compensating.
- Works best for people who sit for long hours, have recurring flare-ups, or want to avoid surgery or medication
- The two-phase approach — foundational stability first, functional strength second — matters more than any individual exercise
- Most people feel meaningful improvement within 4–6 weeks if they follow the correct progression
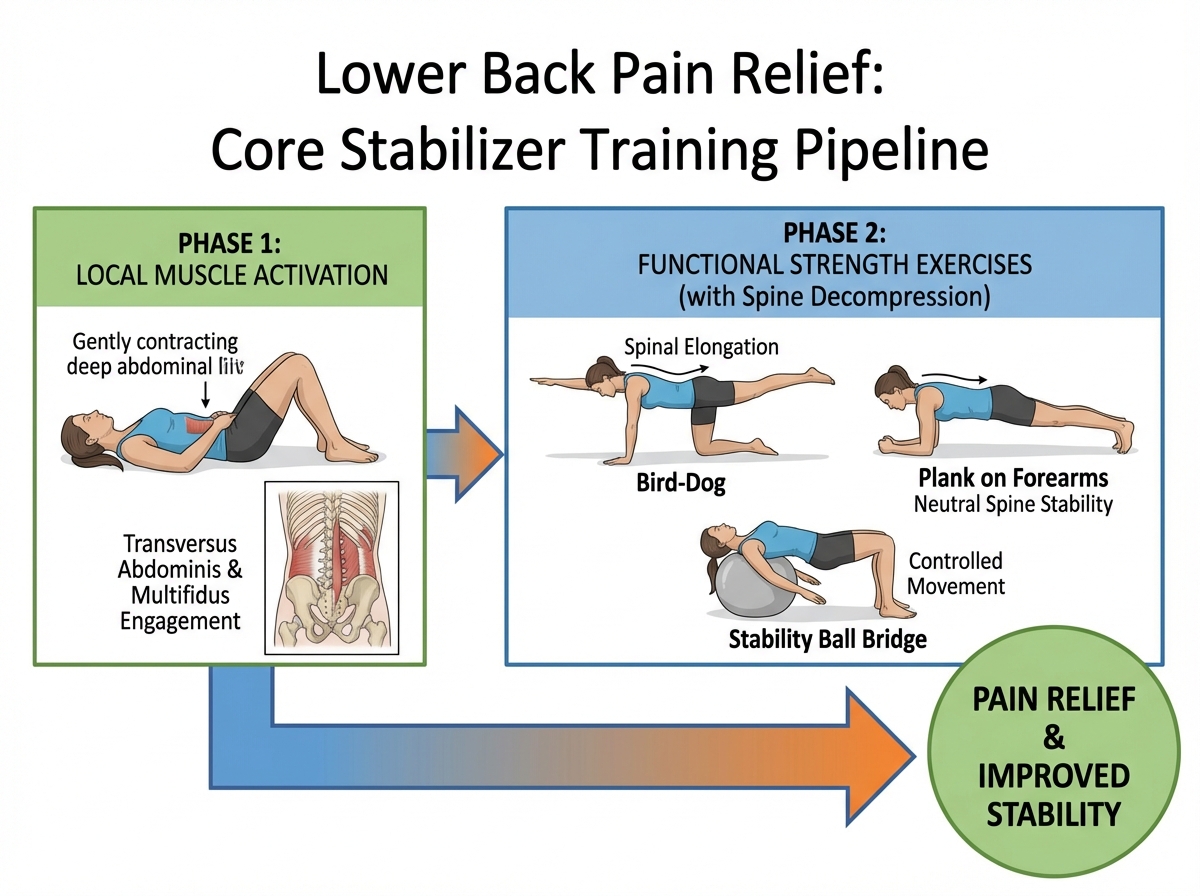
What “Core Stability” Actually Means for a Painful Back
The phrase gets thrown around constantly, but it rarely gets explained clearly for the person who is actually hurting. Core stability, in the context of lower back pain relief, refers specifically to the ability of your deep trunk muscles — the transverse abdominis, multifidus, and pelvic floor — to create a stable base for your spine before any movement happens. These are not the muscles you see in a mirror. They don’t make you look fit. But they are the reason your lumbar vertebrae stay in position when you pick something up, twist, or even just shift your weight while standing.
When these muscles are weak or inhibited, the larger surface muscles — your erectors, hip flexors, hamstrings — try to compensate. They tighten. They overwork. That’s what you’re usually feeling as “back pain.”
| Type | Muscles | Role |
|---|---|---|
| Local stabilizers | Transverse abdominis, multifidus, pelvic floor | Deep spinal support, activated before movement |
| Global stabilizers | Obliques, gluteus medius | Movement control, load transfer |
| Global movers | Erector spinae, rectus abdominis | Power generation, large range motion |
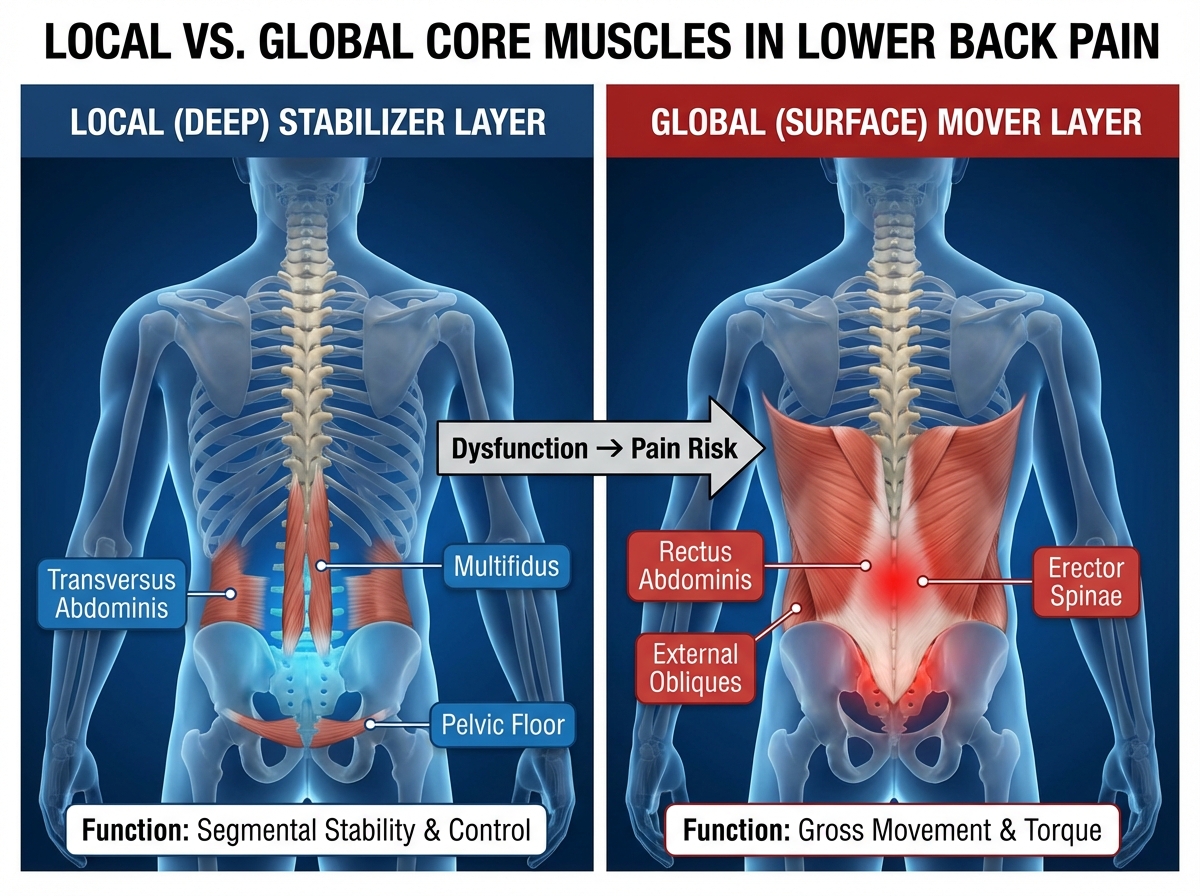
Spine stability doesn’t come from abs alone — it comes from the layer underneath. Tight hamstrings are almost never the root problem; they’re the symptom of something deeper. You can have visible core strength and still have a functionally unstable spine.
How Long Does It Take to Relieve Lower Back Pain with Exercise
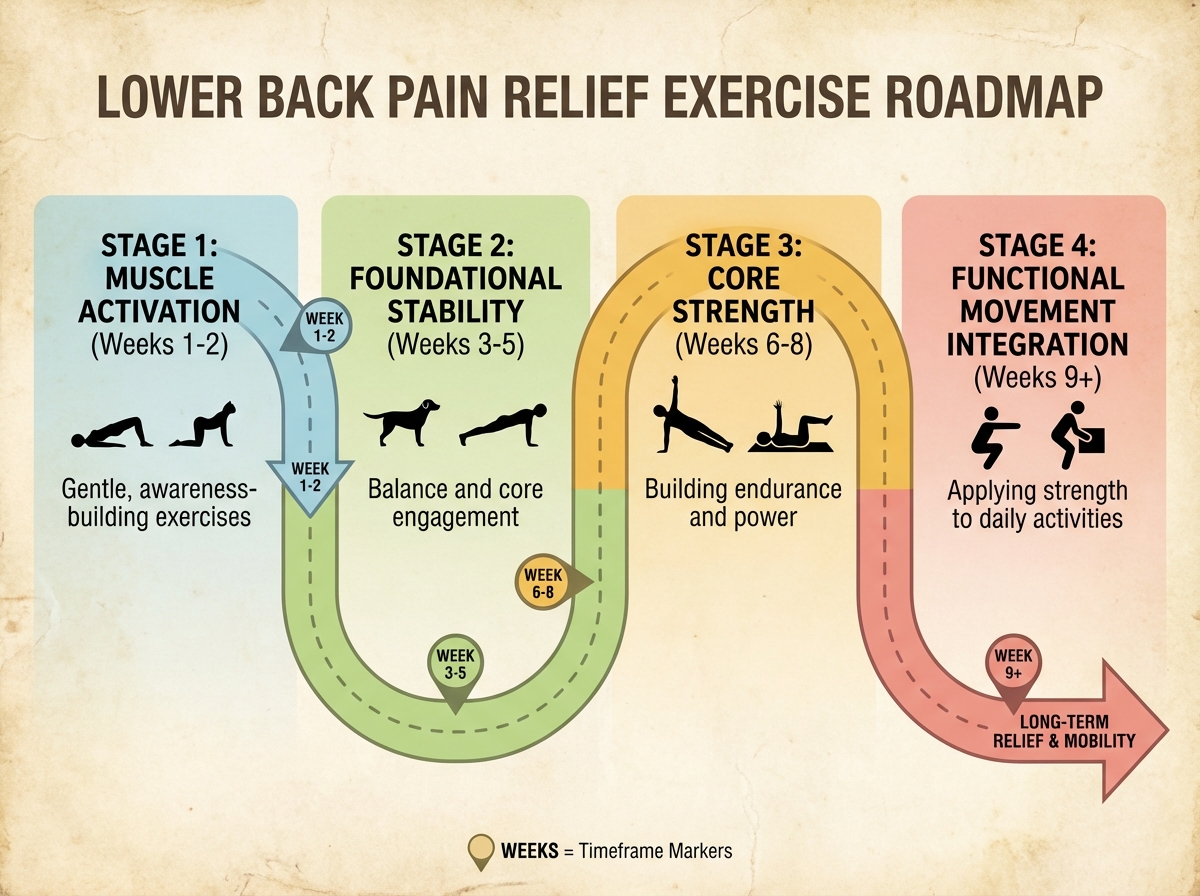
| Stage | Content | Time |
|---|---|---|
| Activation | Learning to consciously engage pelvic floor and deep stabilizers | Week 1–2 |
| Foundational Stability | Basic lying and side-lying exercises, pelvic floor movements with leg raises | Week 2–4 |
| Core Strength | Bridging, ball work, isometric holds, bird dog progressions | Week 4–6 |
| Functional Strength | Standing and loaded movements, lat machine decompression, daily activity integration | Week 6–10 |
| Total | Full foundational-to-functional progression | 8–10 weeks |
The sequence matters more than how fast you move through it — skipping activation to get to “harder” exercises is the single most common reason people plateau. If you take longer than ten weeks, you haven’t failed; you’ve just found that your stabilizers needed more time to come back online, which is more common than anyone admits.
The First Thing You Have to Unlearn
The biggest mistake people make when trying to fix lower back pain through exercise is starting with the wrong layer. They go straight to planks, crunches, or deadlifts because those feel productive. Intensity feels like progress. But the deep stabilizers — the ones that actually protect the lumbar spine — don’t respond to high-load, high-intensity work. They respond to precise, low-load activation. You have to wake them up before you can strengthen them.
The first time you try to consciously contract your pelvic floor muscles while lying on your back, you may feel almost nothing. That’s the point. That absence of sensation is the problem you’re solving. These muscles don’t fire automatically anymore in people with chronic or recurring lower back pain — research consistently shows that the multifidus and transverse abdominis have delayed activation patterns in people who’ve experienced back episodes. The goal of the first phase isn’t to burn. It’s to reconnect.
This is also the phase most people skip entirely, because it doesn’t look like exercise. Lying on your back and raising one leg slowly, or doing small controlled circles with your legs while keeping your pelvis perfectly still — these movements feel almost too simple. They’re not. They’re the foundation the rest of the program depends on.

What Happens When You Start Moving Again
Somewhere in the first two weeks of consistent activation work, something shifts. It’s not dramatic. You might notice that getting out of bed in the morning doesn’t require the same careful negotiation with your spine. Or that you can sit through a meeting without repositioning every twenty minutes. These small changes are significant, because they mean the nervous system has started to trust the area again.
This is also where people make their second big mistake: they feel better and they stop. The pain reduction in the early phase comes from decreased neural sensitivity and a small improvement in muscle activation — not from any structural change. The structural adaptation, the actual rebuilding of stabilizer muscle endurance and coordination, takes six to ten weeks of continued work. Stopping at week two or three because the acute edge is gone means the underlying weakness is still there, and the pain will return.
For people who sit at a desk for most of the day, this phase has a particular quality. You realize that your core has essentially been switched off for hours at a time, every day, possibly for years. The muscles that should be maintaining your lumbar curve have been substituted by your chair back, your hip flexors, and whatever posture you’ve defaulted into. Reactivating them while lying on the floor feels disconnected from your actual daily life — and it is, intentionally. You’re rebuilding the pattern in a controlled environment before you ask it to work under load.
For more on how the body compensates during prolonged sitting and what movement patterns help reverse it, the ideas in how to treat your own back pain and sciatica at home overlap meaningfully with this activation phase.
The Side-Lying and Ball Work Phase That Nobody Talks About
Once basic activation is established — and you’ll know because you can maintain a neutral spine position while moving your limbs without the whole pelvis rocking — the work gets more interesting. Side-lying leg raises target the lateral stabilizers that most people have never consciously trained. They feel easy until you try to do them with true hip abduction, no trunk rotation, and a completely still lower back. Most people discover they’ve been letting their pelvis tilt to compensate on every single repetition.
The ball exercises add an unstable surface, which forces the deep stabilizers to work reactively rather than in a controlled, predictable pattern. This matters because real life — picking up something you dropped, catching yourself from a stumble, twisting to look over your shoulder — is unpredictable. The ball transitions the training from “I can do this movement correctly when I’m focused” to “my spine is actually protected when I’m not thinking about it.”
This stage of core stability exercise for lower back pain is where the work starts to feel meaningful. You’re no longer just activating muscles in isolation. You’re starting to build the coordination between layers — the local stabilizers doing their job while the global movers do theirs, without anyone overcompensating.

When Core Strength Becomes Functional
The transition from stability exercises to functional strength is the most underrated step in the entire process. Most exercise programs skip it entirely — they go from floor work to something like deadlifts or squats, and wonder why the pain returns under load. The functional approach to spinal health means training the spine to maintain stability while the body actually does things: hinging, reaching, rotating, absorbing impact.
Lat machine decompression work is one of the more surprising tools at this stage. Using a lat pulldown machine — not for strength, but as a decompression tool — allows you to gently traction the lumbar spine while the core is actively engaged. The spine gets space. The discs, which have been compressed by hours of sitting or years of poor load distribution, get a moment to breathe. Combined with the strength work, this creates a nervous system signal that the lower back is safe to move freely again.
Athletes with recurring back pain often find this phase the most revealing. They’ve been strong — they have the deadlifts and the squat numbers to prove it — but they’ve been strong with compensations built in. Real functional stability means the deep system and the surface system are working together, not taking turns.

How to Actually Integrate This Into Your Life
The program only works if it becomes habitual, and it only becomes habitual if you make it logistically easy. That means knowing exactly what you’re doing before you start, not figuring it out once you’re already on the floor. It means having a mat in a space where you won’t have to clear room before every session. It means being willing to do ten minutes of activation work on a morning when you only have ten minutes — because ten minutes of the right thing beats nothing.
For people recovering from a period of acute pain, or managing long COVID fatigue, one of the most important clinical insights is that resistance-based core stabilization work does not elevate heart rate. It doesn’t tax the cardiovascular system the way walking or cycling does. This makes it accessible on days when your energy is low and your body is telling you to do less. The how to learn acupressure and pressure point healing as a complete beginner approach to body awareness pairs naturally with this kind of low-load, high-attention training.
The deeper shift isn’t physical. It’s the realization that your back is not fragile. It has been under-supported, under-trained, and over-protected. Movement is not the enemy — the wrong movement, done before the foundation is ready, is the enemy. Once you understand that distinction, you stop fearing the pain and start treating it as feedback.
What to Do Right Now
Start with a pelvic floor contraction test. Lie flat on your back, knees bent, and try to gently contract only the pelvic floor — not your glutes, not your abs. Hold for five seconds. If you feel almost nothing, or if you can’t isolate it, that’s your starting point.
Work on a firm, flat surface. A soft mattress or a thick foam mat will mask the instability you’re trying to correct. Use a thin exercise mat on a hard floor, at least for the activation and stability phases.
Do the basic exercises every day for the first two weeks. Frequency matters more than volume at the activation stage. Ten minutes daily builds the neural pattern faster than forty minutes three times a week.
Add the side-lying leg raises before you progress to any standing or loaded exercise. The lateral stabilizers are almost always the weak link, and skipping them creates a compensation pattern that surfaces later as hip or knee pain.
Use a ball for the instability work only after you can maintain a neutral spine without it. Progressing to unstable surfaces too early just trains your compensation pattern more efficiently — it doesn’t fix it.
If you have access to a lat pulldown machine, use it for spinal decompression at the end of your session. Sit, grip, and let your spine gently lengthen under the weight before you pull. Twenty seconds of decompression after a session of stabilization work changes how your back feels the next morning.
Film yourself doing the exercises once. You will almost certainly discover that what you feel you’re doing and what you’re actually doing are not the same. The pelvis tilts. The lower back arches. Seeing it is worth more than any verbal cue.
Track your morning pain level, not your workout. The real signal that the program is working shows up when you get out of bed — not during exercise. Write it down for six weeks. The trend will motivate you more than any single session.

Leave a Reply